How Do CGMs Work: CGM Accuracy and Tips for Calibration
Key Takeaways
- How CGMs work: Continuous glucose monitors (CGMs) track your individual glucose response by measuring interstitial fluid rather than blood, providing 24/7 data on your metabolic trends.
- BGM vs. CGM accuracy: Blood glucose monitors (BGMs) deliver exact point-in-time values from capillary blood, while CGMs excel at tracking relative glucose changes and overnight patterns.
- CGM calibration requirements: While many modern glucose biosensors are factory-calibrated, you can manually adjust sensor readings by comparing them to a fasting lab value or a reliable glucometer test.
- How CGMs work: Continuous glucose monitors (CGMs) track your individual glucose response by measuring interstitial fluid rather than blood, providing 24/7 data on your metabolic trends.
- BGM vs. CGM accuracy: Blood glucose monitors (BGMs) deliver exact point-in-time values from capillary blood, while CGMs excel at tracking relative glucose changes and overnight patterns.
- CGM calibration requirements: While many modern glucose biosensors are factory-calibrated, you can manually adjust sensor readings by comparing them to a fasting lab value or a reliable glucometer test.
Continuous glucose monitors, or CGMs, are among the most important breakthrough developments in recent biomedical tech. In a nutshell: they're sensors that allow you to track glucose trends 24/7 in a minimally invasive way. Compared with the more conventional blood glucose meters (BGMs), they provide a painless assessment of glucose trends.
Using a CGM is typically as easy as putting it on the right part of your body (more on that later) and letting it track your activity and habits. But before you get started, let’s address the technology itself and discuss how to ensure that you are getting the most accurate readings possible with your new tech.
If you want to make the most of your CGM, it's helpful to know how to use it correctly. This involves learning more about what the device is, how to calibrate it if you ever need to, and what precision and accuracy mean in regards to it.
As with all technology, a CGM has pros and cons, and it’s possible to see minor discrepancies when it functions, which can feel frustrating. Let’s discuss why you might experience this and what you can do about it.
Understanding the CGM

A CGM is a small device you wear on your body that continuously tracks your glucose levels. A CGM has an abundance of benefits, and if you have access to an app like the one Nutrisense offers with its CGM Program, you can track daily activity to see how food, sleep, exercise, and stress impact your glucose.
As a user, you can see 24/7 glucose changes in response to various factors. It shows you how your body responds to these different factors, which can help you optimize your health.
The FDA allows CGM devices and finger-prick devices to have some variation from what you would receive from a blood test at a physician’s office. So, remember, readings from both types of devices can fluctuate! The only way to ensure a perfectly accurate reading is by getting a blood glucose test from a lab.
The most important thing to consider when using a CGM is the relative change in data and the pattern of trends over time, instead of the absolute values or exact numbers. There may be variabilities in absolute value, but CGMs read relative changes in your glucose very accurately.
Think of It Like This
CGM readings are like videos. With the continuous readings, you can get a good overview of how your glucose levels change over time and in reaction to different foods, activities, sleeping trends, etc. We can view trends as opposed to focusing on one specific value.
Finger-prick tests are like a photo of your glucose—they capture a single moment. So, those readings will be based on your choices shortly before pricking your finger.
{{rich-text-cta-3="/style-guide"}}
BGMs versus CGMs: What’s the Difference?

Although BGMs and CGMs are both designed to measure the glucose level in the body, they are not the same. Let's take a look at some of the key differences and advantages of a CGM vs. a BGM.
The Blood Glucose Monitor (BGM)
First of all, BGMs measure the glucose concentration in the blood, which means that it requires finger pricks, leading to local pain and discomfort. BGMs can also only deliver one measurement at a time, making it challenging to identify glucose trends. However, when it comes to absolute values, BGMs are more precise than CGMs.
The Continuous Glucose Monitor (CGM)
The main advantage of CGMs is the ability to measure glucose levels continuously, allowing you to monitor your glucose trends easily. Glucose trend information gives you the power to track the behavior of glucose concentration continually. Also, CGMs, like other continuous glucose monitoring devices like glucose biosensors, don’t require finger pricking, which significantly improves the user experience.
How to Choose Between Them
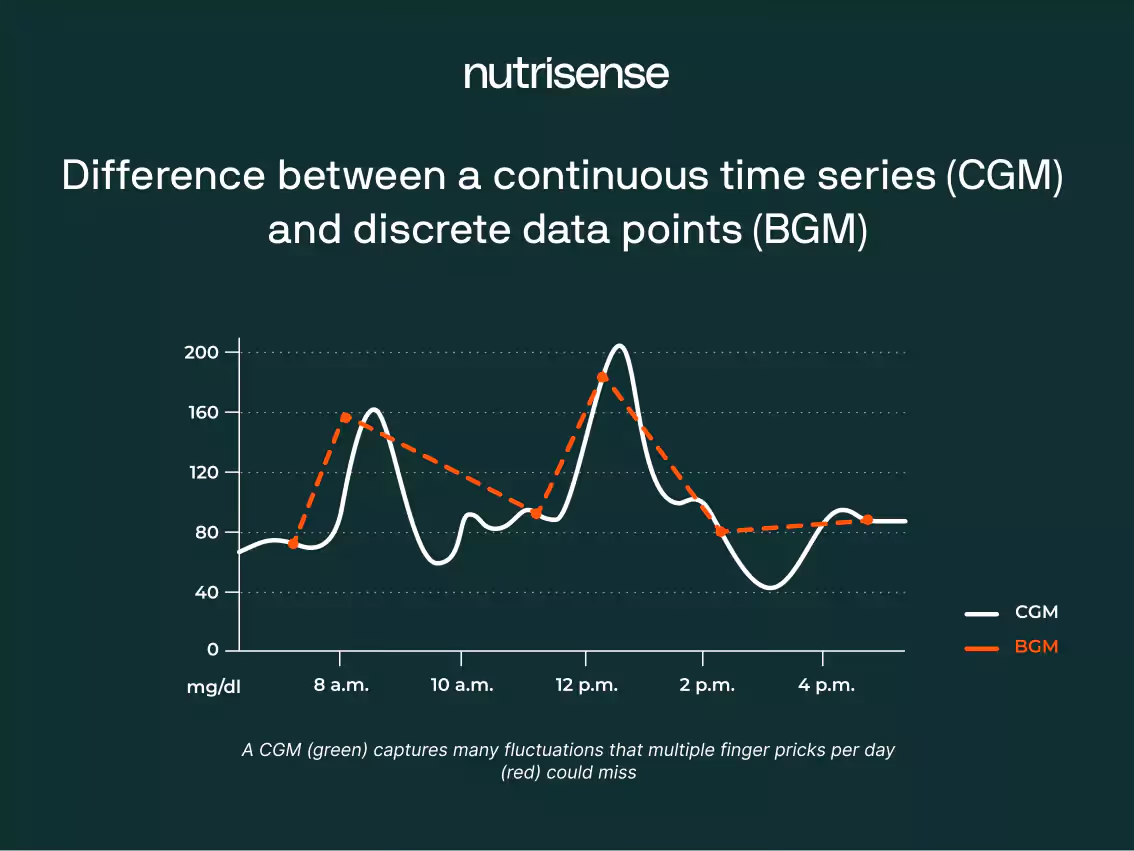
So, which glucose meter is most accurate? CGMs are great to measure glucose evolution over the day, offering 24/7 monitoring in a minimally invasive way. However, when compared with BGMs, CGMs may provide slightly less accurate data with a higher response delay.
This is because sensors measure glucose concentration in the interstitial fluid (ISF), and glucose can take a while to diffuse from the blood to this fluid. So, you can use BGMs when precise glucose measurements are required, while CGMs work best with glucose trend monitoring.
Both measurements are important for health tracking: you can use accurate measurements for diagnostics and device calibration, while glucose trend monitoring can detect sudden spikes in glucose, correlate patient behavior with glucose levels, and help with nutritional decision-making.
Also, it is possible to obtain different measurements from a BGM and a CGM simultaneously, as blood responds faster to glucose variation than the interstitial fluid. A good practice is to measure glucose behavior using a CGM device and then use a BGM sensor to double-check any abnormal readings.
There Are Different Types of CGMs
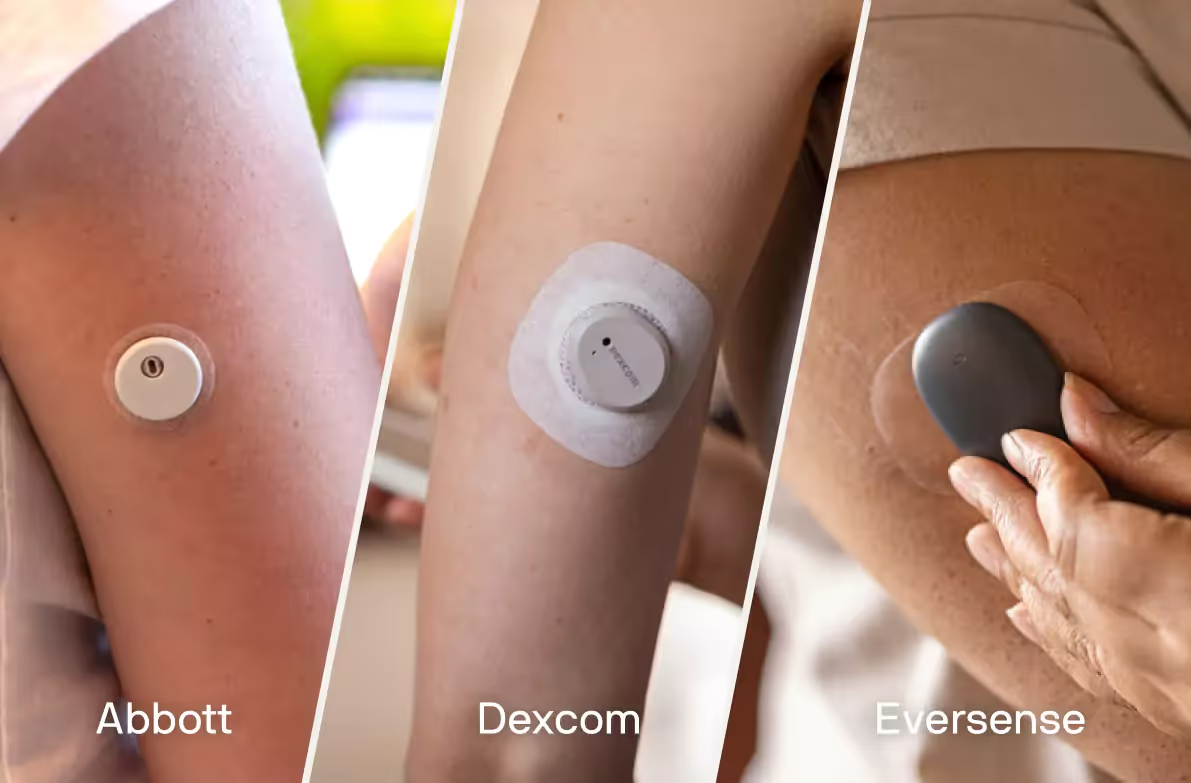
The three most common manufacturers of CGMs are Abbott, Dexcom, and Eversense. The FDA has approved the use of the Freestyle without backup readings from a finger stick device, as it is factory calibrated. There are also now over the counter CGM devices and glucose biosensors that people can choose from.
Now that you know more about the CGM, let's focus on calibration. Both CGMs and BGMs measure the glucose level using electrochemical sensors.
Remember that these sensors have a limited lifespan, so most will have an expiration date. You have to replace the sensor after its expiry date due to a drop in precision.
The second thing to note is that readings can vary because of temperature, body location, manufacturing variations, and other external factors. CGM calibration can help correct these errors by relating the raw readings with actual glucose measurements taken from more reliable techniques. The two main reference methods for calibration are:
1) Using a Lab Value
Laboratory glucose tests use venous blood to measure the glucose level. Venous blood assessment can provide more accurate results due to the higher quality of the sample, with a larger quantity of blood, intact cells, and biomarkers. So, laboratory tests are the gold standard for glucose evaluation.
Here's more about the procedure for lab test calibration:
- Book a lab test with your doctor to test your fasting glucose level.
- Compare your lab value to your fasting (no food for around eight or more hours) glucose reading from your CGM or glucose biosensor in the Nutrisense app.
- If you notice a discrepancy in your CGM reading of around five points or more from the reference lab value, you should try to adjust it. Some sensors allow you to manually calibrate this.
2) Using a Glucose Meter (Finger-Prick)
You can also use a finger-prick glucometer to calibrate your CGM. Although less precise than laboratory tests, finger-prick or fingerstick tests are much more convenient and easier to perform, using just a drop of capillary blood from your finger.
To calibrate your CGM using finger-prick devices, follow these steps:
- Take a fasting (no food for eight or more hours) fingerstick test an hour after waking up before food, coffee, or exercise. Ensure your glucose strips have not expired and that your fingers are clean.
- Compare your reading on the CGM at roughly the same time. Note that there is a 15-45 minute lag between blood glucose and interstitial glucose measurement (which is what your CGM measures).
- During non-fasted times, we need to account for this lag more specifically, but on a fasting comparison, it may not be as necessary. It’s one reason we recommend only making adjustments to the graph in comparison to fasting glucose values when your glucose is most stable.
- As we mentioned above, if you notice a discrepancy in your CGM reading of around five points or more from the reference lab value, you should try to adjust it.
*Remember to wait for 12-24 hours before you decide to calibrate, as your CGM will be using that first day you are wearing it as “warm-up” time.
One thing to consider is the delay between blood glucose readings from a finger stick and the interstitial glucose readings that the CGM reads, as explained in the BGM versus CGM section.
One way to look at it is by using an analogy of a train. Your glucose levels are the train, where the front of the train is the blood glucose reading, which is instantaneous and taken at that moment. At the end of the train is the interstitial readings.
If the train is going up a hill, then the front of the train passes this spot before the caboose, but the caboose still passes by the same spot. So: the two tests take the same reading but with a 15 to 45-minute delay.
What are the FDA Requirements for Commercial CGMs?

At first, the FDA classified CGMs as class III devices, so they were required to pass through a full pre-market approval (PMA) process before release. These included clinical trials and thorough studies about sensitivity and precision. After 2018, however, the FDA defined integrated CGMs (iCGMs) as class II devices, which are cleared from the PMA process and can be approved through the 510(k) submission.
The FDA demands that at least 85 percent of the glucose measurements must have errors lower than 20 percent. What this means is that it’s not unusual to find weird deviations in your CGM device since errors going up to 20 percent in the absolute value can be expected.
The BGM regulation, on the other hand, states that more than 95 percent of the measurements must present errors lower than 15 percent, which is significantly lower than the CGM error. It means that we can expect more precision from BGMs when compared to CGMs.
However, iCGM devices must comply with trend accuracy, which defines how well the device follows a change in the glucose level. This requirement states a maximum error allowed for the rate of glucose change in time. In other words, if your glucose level rises, the CGM measurement value must increase similarly. This change of rate is often more important than absolute values in CGMs since the goal here is to obtain a picture of the evolution of glucose over time.
What CGM Should I Use?
There are currently three major CGM manufacturers: Abbott, Dexcom, and Eversense. They are very similar in terms of the functioning principle. Still, they present some key differences in terms of placement and precision.
The table below compares the wear time, body site, and MARD of a few different devices. MARD stands for Mean Absolute Relative Difference, a metric of statistical dispersion of the CGM measurement and the actual body glucose level. So, if the MARD is large, the statistical dispersion is also large, and, consequently, the precision is low.

We can see that the measurements are similar for the three CGMs, so the advantages come from the device specifications. For instance, some glucose biosensors available over-the-counter will likely have the lowest price per sensor.
In contrast, the Eversense has the longest wear time. However, the Eversense CGM requires surgical insertion and removal, significantly more invasive than its counterparts.
Another note is that these studies compared the CGMs with the Dexcom G5. The most recent market version of the Dexcom prescription-only CGM is the G7 version, which provides factory calibration, a 10-day wear period, and an overall MARD of nine percent [2]. There are also newer devices on the market, including the Stelo Glucose Biosensor, a great over-the-counter option especially when paired with expert guidance to help you understand and action the glucose data.
Location Matters

The application site of the CGM sensor varies by manufacturer. Still, they are usually restricted to the upper arm and the abdomen. It's because the biochemical structure of the body, such as the fat and muscle percentage and water content, changes with the location, including the interstitial tissue used to detect glucose. For instance, a CGM placed on your foot will give different readings from a CGM on your upper arm.
Since the manufacturer expects the CGM to be on the recommended location, especially in factory-calibrated devices, improper placement can cause issues. Different sites on the same person can give different absolute readings. Studies have even found variations between the left and right arms.
Since most commercial CGM devices are FDA-approved only for specific locations, following the manufacturer’s instructions for the application site is crucial to get the best performance from your CGM.
There May Be Other Reasons You’re Getting an Abnormal Reading

You may notice a spike in your CGM reading that seems out of place and may appear to be an error on the technology’s part. There are a few reasons this could be happening—and it’s not because your CGM is broken or unreliable!
1) Your CGM is Inserted into a Muscle
People who are very lean with little body fat often have to manually calibrate the sensor to a greater degree than others. The probe in the sensor needs to be completely bathed in interstitial fluid. While this may affect the absolute calibration, it will not affect the relative changes in glucose levels over time.
2) You Take High Doses of Vitamin C
High doses of vitamin C can cause a “false spike” in your data. Vitamin C affects your interstitial fluid and not your blood glucose levels in this case. If you think you may be able to decrease your dose of Vitamin C, speak with your doctor.
3) You Take Certain Medications
Drugs like Tylenol/acetaminophen can also cause a false spike. It’s due to the acetaminophen’s interaction with the electrodes in your CGM. Remember that if you take higher doses of this medication, you may see higher spikes from two to eight hours after ingestion.
If you aren’t sure what might have caused a given glucose response, reach out to a specialist. The registered dietitians and nutritionists at Nutrisense are glucose-certified and trained to help you troubleshoot these situations.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
How accurate are CGMs compared to BGMs?
The main difference in BGM vs. CGM accuracy is that BGMs deliver exact point-in-time values, while CGMs track continuous glucose trends. A continuous glucose monitor measures interstitial fluid rather than capillary blood, causing a slight physiological delay during rapid shifts. However, this 24/7 data is highly accurate for identifying your individual glucose response and metabolic patterns.
What are the different types of CGMs?
The main types of continuous glucose monitors include over-the-counter glucose biosensors, prescription-only devices, and long-term implantable sensors. Major manufacturers like Abbott (makers of Freestyle Libre and Stelo), Dexcom, and Senseonics (Eversense) offer devices that vary in wear time, sensor placement, and calibration requirements. Choosing the right CGM depends on whether you need it for medical management or general metabolic optimization.
Should I use a glucometer to calibrate my CGM?
Calibration depends on your specific continuous glucose monitor and whether you notice discrepancies during fasting periods. While many modern glucose biosensors are factory-calibrated, you can use a high-quality glucometer reading taken first thing in the morning to manually adjust your CGM data if it drifts more than five points from a reliable baseline.
How do you switch from a BGM to a CGM?
You switch from a BGM to a CGM by applying a wearable sensor to your arm or abdomen instead of relying on daily finger pricks. Because a continuous glucose monitor tracks 24/7 data, you gain visibility into overnight patterns and post-meal spikes that isolated blood tests miss. Working with a Registered Dietitian helps you interpret this continuous data to build a personalized metabolic strategy.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Amanda is a Nutrition Manager and Registered Dietitian, with a Masters in Dietetics from Stephen F. Austin State University. Originally from south GA, she got her undergrad degree from Texas Tech University. She worked at a hospital in Fort Worth, TX, for 4 years as a dietitian, counseling those living with HIV.



.avif)
