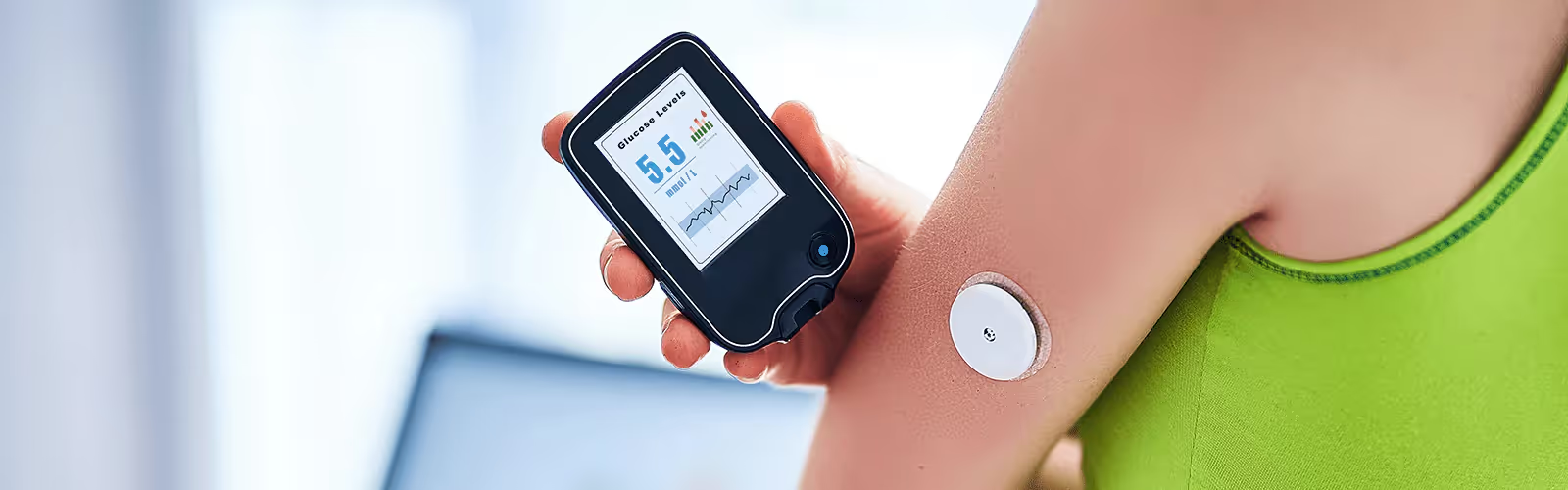
How to Check Blood Sugar at Home Without a Meter: 3 Ways

Key Takeaways
- Checking glucose without a meter: The most reliable alternative to a traditional finger-prick glucometer is a continuous glucose monitor (CGM), which measures interstitial glucose levels via a wearable sensor.
- Testing without pricking your finger: CGMs eliminate the need for daily needles, giving you 24/7 data on your individual glucose response through a connected app.
- At-home glucose monitoring: Tracking your levels at home helps you understand how specific foods, sleep, and lifestyle habits directly impact your energy and metabolic health.
- Checking glucose without a meter: The most reliable alternative to a traditional finger-prick glucometer is a continuous glucose monitor (CGM), which measures interstitial glucose levels via a wearable sensor.
- Testing without pricking your finger: CGMs eliminate the need for daily needles, giving you 24/7 data on your individual glucose response through a connected app.
- At-home glucose monitoring: Tracking your levels at home helps you understand how specific foods, sleep, and lifestyle habits directly impact your energy and metabolic health.
The advances in health technology have made it much easier for people to get real-time insights into their blood glucose, or blood sugar, levels. But testing and monitoring your glucose levels itself isn't new. The first diagnostic test for diabetes was created as far back as 1841. It analyzed glucose levels by analyzing urine using acid hydrolysis, a test that breaks down larger molecules such as glucose into smaller ones.
Over the following centuries, scientists refined this urine analysis method further by using different compounds. But it wasn’t until the 1970s that glucose blood tests such as the hemoglobin A1c, or HbA1c, became available.
Eventually, at-home finger-prick tests became available for use by the general public. Nowadays, technology has made it even easier to get 24/7 glucose level analysis without needing to prick fingers every time. You can now use tools like the continuous glucose monitor to track glucose in real-time.
Read on to learn how glucose testing and self-monitoring has made it easy for people to maintain normal blood glucose levels.
Why You Should Check Your Blood Sugar by Monitoring Glucose Levels
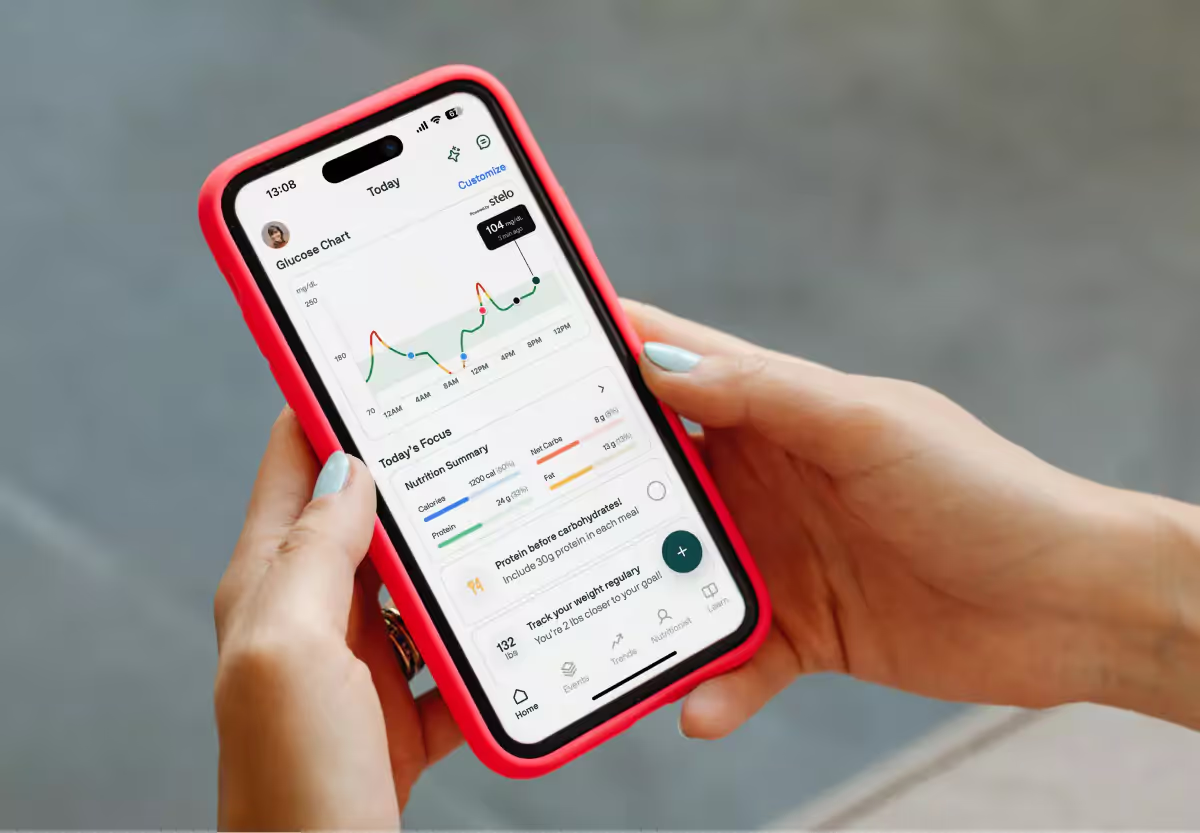
Blood glucose levels constantly fluctuate as you eat, exercise, and sleep. To get accurate insight into your glucose levels, you’ll want to start monitoring them throughout the day.
While HbA1c testing every few months can be necessary, monitoring your levels on a more regular basis can improve your habits and optimize your health. Let’s dive into how checking your blood sugars on a more regular basis does that.
Monitoring Glucose Reduces HbA1c In Type 1 and 2 Diabetes
You may already be aware that self-monitoring glucose levels is supposed to help. But did you know that continuous glucose monitoring can be even more beneficial than the standard finger-prick method?
One study found that self-checking glucose levels using a continuous blood glucose monitor significantly reduced hemoglobin A1c or HbA1c compared to standard glucose testing in the management of those with type 1 diabetes. Researchers have found similar benefits for type 2 diabetes management.
This may be due to 24/7 data on glucose levels allowing you to see what foods your body reacts well to. It also becomes easier for you to connect the dots and learn (from the trends in your glucose data) how to better manage your levels.
While CGMs and glucose biosensors don't check blood glucose, they do measure glucose in the interstitial fluid, which gives you an idea of how your body is using sugar. They require less attention from the user—some require minimal scanning while most modern versions are Bluetooth-enabled and sync automatically. With most sensor models, you can have access to your glucose levels continually. With a glucometer or finger-prick method, you may forget or feel aversive to pricking your finger multiple times a day.
Researchers also describe that continuous glucose monitoring can allow people to measure silent hypo or hyperglycemia (where you don’t feel any symptoms, but your glucose levels are still imbalanced).
Regardless of if you are using standard glucose testing at home or a continuous monitor, regular self-monitoring can be beneficial for improving HbA1c and managing diabetes.
{{rich-text-cta-3="/style-guide"}}
Monitoring Glucose Helps Optimize Energy Levels
Glucose, a sugar molecule, is your body’s primary energy source. Every cell in your body can run on glucose and use it in various functions. Insulin is the hormone that signals your cells to let the glucose in to be used for energy or stored for later use.
Things can go awry when insulin production or signaling isn’t working correctly. There may be too much glucose in the blood when this happens, and you may experience symptoms like fatigue, headaches, and/or brain fog.
Certain foods can and will lead to blood sugar spikes which may result in a subsequent drop, making you feel like you had an energy crash.
Monitoring your glucose may help you understand what foods on their own or in combination, may keep you energized throughout the day and which create these energy fluctuations throughout the day. You can then use this info to make eating decisions that are best for you.
Understand How Lifestyle Can Impact Glucose Levels

Similarly to getting insight into how certain foods impact energy levels, you can start to understand how your lifestyle choices affect glucose levels too.
If you’ve had a hunch that stress leads to blood sugar spikes and crashes, you can test the theory by self-monitoring glucose levels.
And then, you can use the data to optimize your lifestyle habits.
Seeing the impact your habits have will also encourage you to stick to them. You may notice long-term improvements in glucose levels, insulin sensitivity, and weight management with healthier habits.
Can You Monitor Your Blood Sugar Without a Meter?
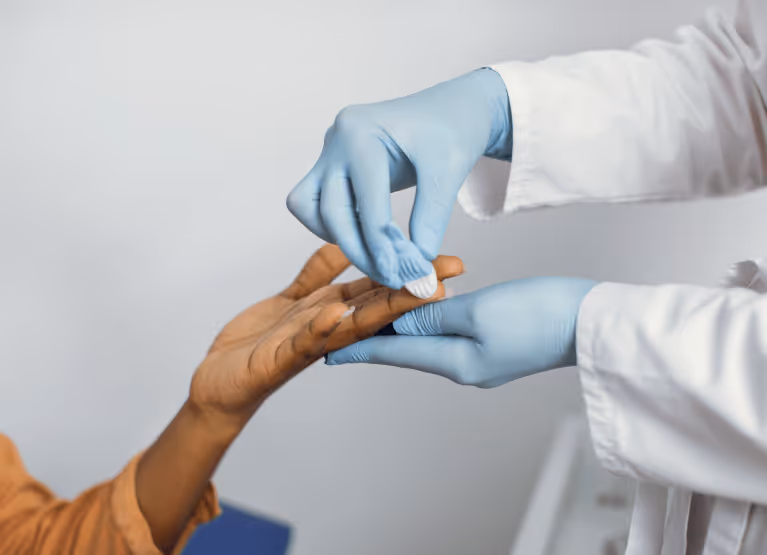
Not exactly. The most widely known method of checking blood sugar is using the finger-prick method with a glucometer. If you’re not familiar, this method involves pricking your finger using a lancet.
Once pricked, you can place the drop of blood on a strip. The strip is then inserted into a meter that measures the amount of glucose attached to your blood cells.
We’ve already alluded to this, but — thanks to modern technology — you don’t have to prick your finger every time you want to check your glucose levels.
Different Ways to Check Your Blood Sugar
Here are scientifically-backed alternatives to monitor your blood sugar. Some may be more helpful than others. However, you should choose the method that best works for your needs. And you can always discuss these options with your doctor.
Common Alternatives to the Finger Prick Method
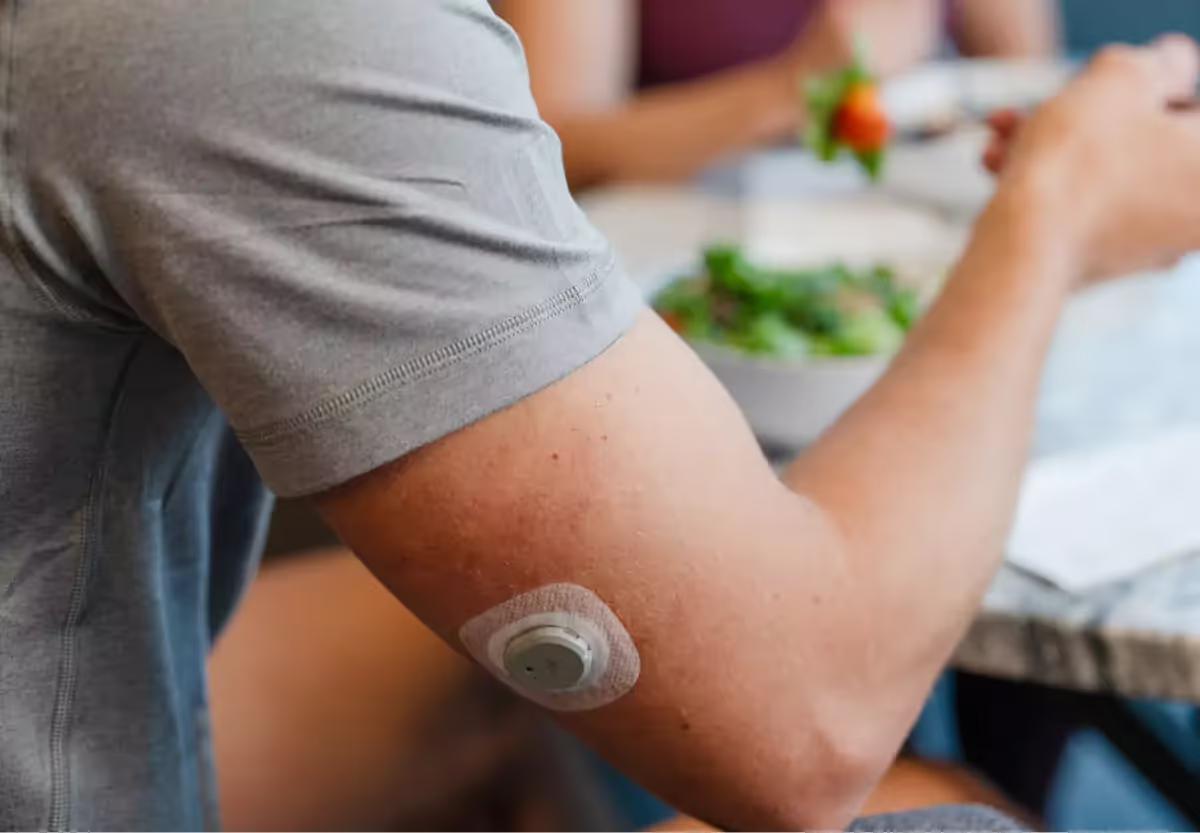
1) CGMs or Glucose Biosensors
A continuous glucose monitor (CGM) or glucose biosensor, is a sensor placed on your skin (most commonly on your arm), with a patch on top to protect it. These sensors directly measure glucose levels.
While the standard glucometer test measures the amount of glucose attached to red blood cells, a CGM or glucose biosensor measures interstitial glucose levels.
Usually, the patch stays attached, and the device measures your glucose levels continually—even as you sleep. It gives you 24/7 data on how your glucose levels fluctuate as you eat, sleep, and do your daily activities.
2) FreeStyle Libre 3, Dexcom G7 and others
The FreeStyle Libre 3 and Dexcom G7 are a specific type of CGM monitor—a discrete patch with a painless sensor attached. The latest models are Bluetooth-enabled and automatically sync to read your glucose levels. Once integrated with an app like the Nutrisense App, you can start understanding your data to reach your health goals.
3) Urine Test
Urine testing for glucose levels is rarely done anymore, as better methods have become available. This type of testing involves using a dipstick to measure the amount of glucose present in the urine.
Understanding Your Blood Sugar Levels
Normal blood sugar levels can range from 70 to 99 mg/dL. However, optimal blood sugar levels will look different for different people.
The Nutrisense Nutrition Team generally recommends daily average glucose of <105 mg/dL for a healthy individual, with fasting values between 70-90 mg/dL. It’s also best to avoid repeated spikes of >140 mg/dL.
Working with a credentialed, glucose-certified dietitian or nutritionist alongside a healthcare professional can help you understand what optimal glucose levels look like for you, and prevent very high or very low glucose levels.
Dangers of Lower Blood Sugar Levels
Hypoglycemia, or low blood sugar, is when your blood sugar levels are below normal. Because glucose is the body’s primary energy source, hypoglycemia is extremely dangerous and can be fatal if it’s not addressed.

If you detect any of the signs of hypoglycemia, you should first consume 15 grams of easily digestible carbohydrates. It can be in the form of juice, sugar, or glucose tablets.
Focus on consuming simple sugars with low fiber instead of fiber-rich complex carbohydrates. Then recheck your blood sugars 15 minutes later to see if you have normalized.
If you have, eat a small snack containing mostly protein to stabilize your glucose levels. If your levels are still low, repeat with another 15 grams of easily digestible carbohydrates and retest accordingly.
Dangers of Higher Blood Sugar Levels
On the other hand, having consistently high blood sugar levels or hyperglycemia can be damaging to your health as well. Hyperglycemia can create inflammation, lead to weight gain, and leave you feeling lethargic and not your best.

When to Reach Out for Help
In addition to some of the symptoms mentioned above, seek the help of a medical professional if you experience the following:
- Drowsiness
- Disorientation
- Extreme dizziness
- Falling unconscious
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
How can I check my blood sugar at home?
You can check your glucose at home using a continuous glucose monitor (CGM), a standard glucometer, or a urine dipstick test. A CGM works by measuring interstitial fluid through a wearable sensor, giving you 24/7 data on your individual glucose response. This method allows you to track trends without needing clinical lab visits.
Can you test blood sugar without pricking your finger?
Yes. Continuous glucose monitors track your levels using a small, wearable sensor instead of daily finger sticks. This provides a painless way to gather 24/7 data on how your lifestyle and diet choices impact your metabolic health over time.
How do you test blood sugar without blood?
You can test glucose without a direct blood sample by using a continuous glucose monitor (CGM) or a urine test. CGMs measure glucose in your interstitial fluid—the fluid surrounding your cells—rather than your bloodstream. While older urine tests are also bloodless, they are significantly less accurate than modern biosensors.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Natalie received her degree in Dietetics from Mansfield University and a Master’s in Clinical Nutrition from the University at Buffalo. Her career has included nutrition education and program development in her local community, adjunct faculty at several collegiate institutions, and clinical nutrition in both inpatient and outpatient settings.